What We Do
The FlexScripts Advantage
FlexScripts takes pride in being an advocate for employers trying to manage their employee benefit prescription drug costs. We provide our clients with our contract expertise and audit services to confirm their contract guarantees are being met.
FlexScripts also Negotiates Contracts, Optimizes Formularies, Provides Independent Clinical Solutions & Cost Saving Strategies to assure our clients have the most competitive PBM pricing.


Self-Funded
FlexScripts works primarily with self-funded employer groups.
FlexScripts Administrators offers a unique pharmacy benefit program to its broker partners and clients. FlexScripts takes pride in managing pharmacy benefit spending for brokers and their clients. FlexScripts leverages their book-of-business and PBM contracting expertise to get maximum value and the most competitive PBM contract pricing.
PBM Contract Guarantees
The FlexScripts program offers market-leading pricing within a true transparent contract. As part of this unique offering, FlexScripts holds our PBM partners accountable by auditing contract & rebate guarantees to confirm the PBM is meeting the terms of their contract. FlexScripts is your clients’ advocate.


PBM Auditing
FlexScripts continuously audits the claims administration process to ensure that both contract pricing and plan design are properly administered by the PBM. We ensure that every dollar an employer spends on their employee pharmacy benefit is being spent in the most cost-effective manner.
Our audits can provide insight into how the PBM is performing based on their contract guarantees and we can notify the PBMs to correct their pricing should they fall short in any quarter. This ensures that no matter what size our clients are, they are receiving the pricing guarantees as promised within the contract.
Specialty Advocacy Programs
In today’s changing market the need for additional oversight and assistance on high cost Specialty medications is essential to save our clients’ money. FlexScripts has partnered with two unique organizations that provide members and plans significantly reduced costs for specialty and high cost medications.
These programs review the current financial situations of each member as well as independently negotiate the cost of the medication with each drug manufacturer. These programs can be used in conjunction with the current PBM plan to provide the best possible options in plan and member adherence and savings.


International Pharmacy & Co-Pay Assistance Programs
FlexScripts uses several trusted & well-known International Pharmacies to ensure that we are getting the best possible pricing on Brand name & Specialty drugs for our clients. Flex works with our PBM partners to bypass rebates and guarantee the lowest Net Cost for our clients.
Co-pay card programs offered by drug manufacturing companies are a direct way to lower out-of-pocket costs for prescription drugs for eligible patients. The cards can enable patients to afford the preferred medications. The adjudication process involves taking advantage of member cost share & plan paid amounts to save additional money for our clients.
Formulary Management
FlexScripts will work with each individual employer group to determine what drugs and policies they want followed to best serve their companies and their members needs.
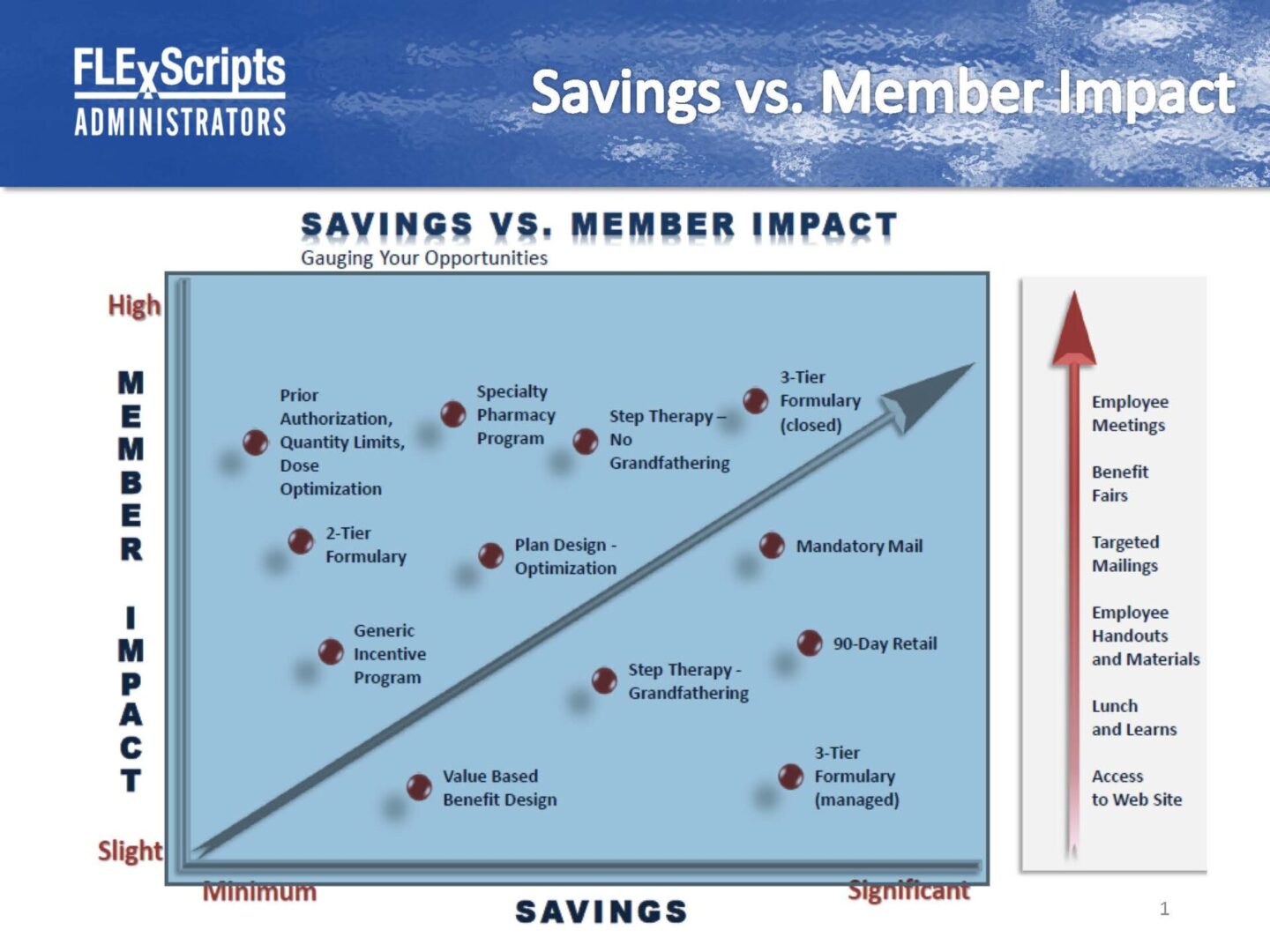
We work on a Savings verses Member Impact scale and can adapt our formulary management to whatever fits each companies needs.

Prior Authorizations
FlexScripts clinical team manages prior authorizations and ensures that our clients are taking the correct drugs for the right afflictions per FDA guidelines. They also make sure our clients are taking the prescribed dosages and adhering to the doctors' prescriptions.
Infusions/J-Code Solutions
FlexScripts has the ability to put plans into place that recognize J-Codes before they process through the medical side. We can recognize the J-Codes/Infusions and process them through the Pharmacy side, which allows us the control to negotiate rates to save our clients millions of dollars.
Some of these infusion sights charge hundreds of thousands of dollars to administer these high cost medications, we negotiate this process and have our infusion centers administer these drugs at our facilities or at client homes and save those astronomical costs.


RFP - Market Intelligence
FlexScripts offers a "PBM Checkup Report" along with our built-in RFP that we have perfected over years of industry experience. We have already vetted many of the PBMs around today and have contracts with the best in the industry. FlexScripts combined services eliminates the need for an RFP, an audit or a dedicated pharmacy consultant. On average, pharmacy consultants will charge $25K for an RFP, $25K for an audit & up to $15K for consulting services. FlexScripts eliminates this expensive charge and offers one of our pre-negotiated PBM contracts of the client’s choosing. Our fee is a flat dollar amount usually offered on a per claim basis. We expose ALL revenue streams within the PBM, TPA and any Consultants to offer complete transparency within the current contract. FlexScripts' assists with this entire process while also removing the black box pricing and games played within the contract. We are the "PBM Police" and we will fight for our clients' best interest every time!
Plan Design Optimization
FlexScripts’ independent consultant review of the clients’ overall plan design allows for a personalized assessment and recommendations. This individualized assessment controls costs in the long-term as well as allowing flexibility to implement any type of plan design.

